Due to the systemic nature of inflammation in inflammatory bowel disease (IBD), the disease can affect more than just the gastrointestinal system. These symptoms are known as extraintestinal manifestations (EIM). Up to 50% of patients experience these manifestations, with skin manifestations being the two most common, along with joint and ocular manifestations.
News
IBD ASSOCIATED DISEASES
July 1, 2025
News

Between 6% and 47% of people with these diseases have been found to have symptoms outside the gut as well: 43% of patients with Crohn’s disease or 31% in those with ulcerative colitis. There may be percentage differences depending on the ethnicity or race of the patients or the geographical area of study.
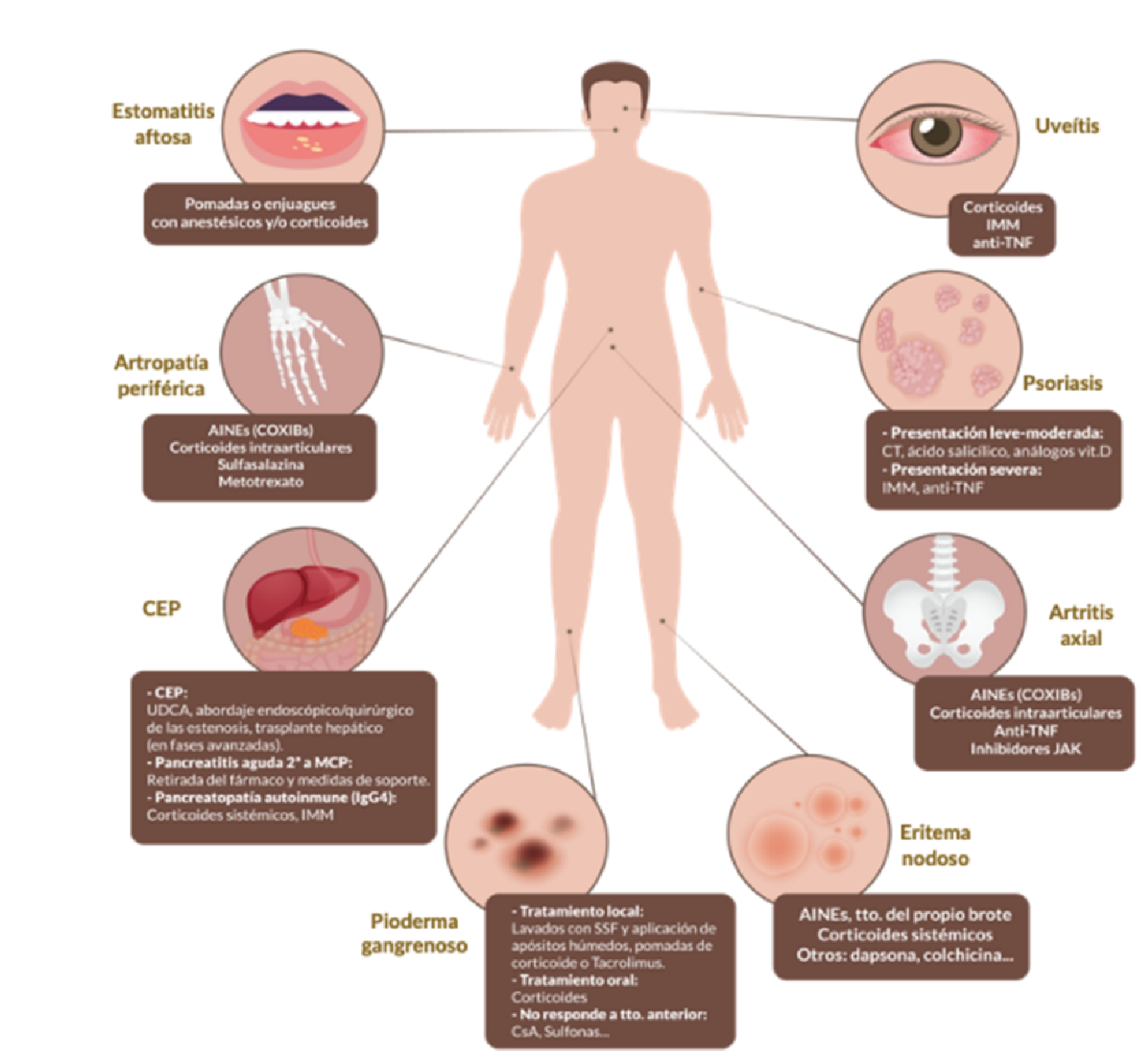
Sometimes these symptoms manifest themselves before IBD is diagnosed, even up to five months earlier in more than 10% of patients. This point is of utmost importance as dermatological and ocular manifestations are visible on inspection and can therefore alert the relevant specialist to the possibility that the patient may develop intestinal symptomatology early on and reduce diagnostic delay and treatment.
It has also been shown that the development of one EIM appears to increase the susceptibility to develop others.
The occurrence of EIM complicates the management of patients suffering from IBD and often requires a multidisciplinary approach, which is widely recommended by scientific societies
1 – Eye Manifestations

.
.
IBD can cause problems due to inflammation that affect the whole body, including the eyes.
In addition, stress, nervous system disorders or some medications (such as corticosteroids or immunosuppressants) can cause or worsen these eye problems.
They occur in less than 5% of IBD patients.
What eye diseases can occur?
- Uveitis:
- Inflammation of the middle inner part of the eye.
- Can cause pain, redness, sensitivity to light and loss of vision if left untreated.
- Episcleritis:
- Mild, superficial inflammation.
- Causes redness but no visual damage.
- Scleritis:
- Deeper and more painful inflammation that can affect eyesight.
- Dry eye syndrome:
- Lack of tears or rapid evaporation, leading to discomfort and burning.
- Keratopathy:
- Affects the cornea.
- Can cause blurred vision and eye pain.
To prevent these symptoms from occurring or, if they do, to minimize their impact, we should have regular eye check-ups, look out for redness, pain and blurred vision, manage stress and take care of our gut, take supplements such as curcumin and seek help if symptoms occur.
2 – Skin Manifestations

Skin manifestations are quite common in people with IBD, appearing in 13-14% of patients throughout the course of the disease.
Although they are more common in people with ulcerative colitis or Crohn’s disease, the lesions vary depending on the type of diagnosis.
There are several types of skin lesions in IBD:
- Those directly associated with IBD: Related to chronic inflammation, typical in Crohn’s disease, e.g. erythema nodosum or cutaneous Crohn’s disease.
- Lesions due to immune dysfunction: occur when the immune system is disturbed: Psoriasis or vitiligo.
- Lesions secondary to treatment or malnutrition: acne, stretch marks, eczema or increased risk of skin cancer.
The main dermatological manifestations are:
- Erythema nodosum:
- This is the most common, affecting approximately 4% of patients, mainly young women with Crohn’s disease.
- These are painful red-violaceous nodules on the legs (thighs, ankles and legs).
- They improve with IBD treatment.
- Pyoderma gangrenosum:
- More common in patients with ulcerative colitis, starting as a pustule and developing into a painful ulcer.
- Usually appears on the abdomen, thorax and/or legs, arms.
- It may appear after a trauma or surgery.
- Requires local treatment and intake of corticoids or immunosuppressants.
- Psoriasis:
- Affects 7-11% of IBD patients, as it is genetically related to IBD, especially in CD.
- They share genetic factors, chronic inflammation and alterations in the intestinal microbiota.
- Some treatments for IBD can cause psoriasis.
- Aphthous stomatitis:
- These are painful ulcers in the mouth, very common in patients with any IBD.
- They improve with control of intestinal inflammation.
- Some treatments for IBD can cause psoriasis.
- Concomitant vasculitis:
- inflammation of blood vessels that may manifest on the skin as red-violaceous lesions of variable size and are usually not painful.
- It can develop into a more serious condition if left untreated, and patients with this condition should seek prompt medical or emergency care.
- Sweet’s syndrome (SS)
- sudden onset of red or purplish bumps on the body, accompanied by fever, headache, joint pain and fatigue.
- usually follows symptoms of intestinal inflammation in IBD, (if the patient experiences a flare-up, SS bumps may begin to appear on the skin).
3 – Osteoarticular Manifestations

Joint manifestations are the most common in people with IBD, with an incidence in people with IBD of 30-35%.
Exercises such as Pilates, yoga, swimming or passive stretching are recommended to prevent them or improve their symptoms, as well as taking certain anti-inflammatory drugs such as COX-2 inhibitors.
- Peripheral arthritis:
- It is the most common, affecting approximately 1 in 4 patients (20-25%), mainly women.
- Painful inflammation of the joints, mainly in the knees, wrists, elbows and fingers.
- Ankylosing spondylitis:
- More common in men
- Affects the spine.
- Manifests itself with low back pain and morning stiffness.
- Sacroiliitis:
- It is also very common (14%)
- Inflammation of the sacroiliac joint (pelvis)
- Presents with pain in the lower back and radiates to the upper thigh.
- Osteoporosis:
- Very common, affecting 30-50% of patients.
- Corresponds to a loss of bone mass
- Risk factors may be: advanced age, family history, medication such as corticoids, or habits such as smoking or alcohol.
4 – Other IBD- associated diseases
Neurological manifestations
- chronic headaches.
- severe fatigue.
- peripheral neuropathies.
Hepatic and biliary complications
- Primary sclerosing cholangitis: chronic inflammation of the bile ducts.
- Fatty liver disease.
- Autoimmune hepatitis.
Cardiovascular and respiratory manifestations
- Increased risk of deep vein thrombosis and pulmonary embolism.
- Increased risk of cardiac disease in severe cases.
Nutritional complications
- Neurological manifestations
- chronic headaches.
- severe fatigue.
- peripheral neuropathies.
- Hepatic and biliary complications
- Primary sclerosing cholangitis: chronic inflammation of the bile ducts.
- Fatty liver disease.
- Autoimmune hepatitis.
- Cardiovascular and respiratory manifestations
- Increased risk of deep vein thrombosis and pulmonary embolism.
- Increased risk of cardiac disease in severe cases.
- Nutritional complications
- Anaemia: due to lack of iron, vitamin B12 or folic acid.
- Vitamin D, calcium or zinc deficiencies.
- Weight loss or malnutrition.
- Vitamin D, calcium or zinc deficiencies.
- Weight loss or malnutrition.
1.-Hernández, V., & López-Sanromán, A. (2019). Manifestaciones extraintestinales de la enfermedad inflamatoria intestinal. Revista Médica Clínica Las Condes, 30(6), 571–580. https://doi.org/10.1016/j.rmclc.2019.06.005
2.-EducaInflamatoria. (s.f.). Manifestaciones extraintestinales. EducaInflamatoria.com. Recuperado de https://educainflamatoria.com/category/manifestaciones-extraintestinales/
3.- Grupo Español de Trabajo en Enfermedad de Crohn y Colitis Ulcerosa (GETECCU). (s.f.). Otras enfermedades en la colitis ulcerosa. Recuperado de https://geteccu.org/contenidos/up/2015/07/Otras-enfermedades-CU.pdf
Contact UsFor more information
Contact Us